| |
Glaucoma is a "silent
killer" or like "slow poison". In most cases it
begins un-noticeably and damages the eyes without
any sign or symptom till it is very late and the
patient is almost at the verge of blindness. This is
the reason that awareness about glaucoma and its
treatment is important to prevent this blinding
disease. |
 |
What is it? |
| |
The contents of the eye-ball are under some pressure (intra-ocular pressure) which maintains the shape of the eye. In certain situations this pressure may rise and be detrimental to the functioning of the nerve of the eye (optic nerve). This is called Glaucoma.
Normal Intraocular Pressure 11 - 21 mm Hg
Rarely, pressure may not be increased but still damage to the optic nerve occurs because of its increased vulnerability, this is called normal tension or low tension glaucoma. |
 |
What are the types of Glaucoma? |
| |
There are 2 main types of glaucoma:
Open Angle Glaucoma
Angle Closure Glaucoma
The fluid of the eye (aqueous) circulates through anterior chamber and passing through the angle exits from the eye into the Canal of Schlemn. In open angle glaucoma the passage to the canal of Schelmn offer resistance to the flow of aqueous . In angle closure glaucoma the angle of the chamber is narrow or gets closed preventing the drainage of aqueous from the eye. Both the situations lead to increase in intraocular pressure. |
 |
How does it lead to blindness? |
| |
Increase in pressure
in the eye leads to resistance to flow of
blood into the eye leading to damage to
vulnerable parts especially the optic nerve which
carries the visual signals to the brain.
First it leads to damage to some areas of
visual field (the extent of surrounding
visible to any one eye). This field loss
progresses gradually till the eye is
completely blind. Early field loss can be
detected by test called Visual Field
Examination or Perimetry. |
 |
Who are the people at risk of
developing Glaucoma? |
| |
Following are the
risk factors for Glaucoma:
-
Family history
of glaucoma (especially in parents and
siblings)
-
Refractive
errors (Myopia or Hypermetropia)
-
Diabetes
mellitus
-
Thyroid Diseases
-
Injudicious use
of steroids especially steriod eye
drops.
-
Certain eye
conditions e.g. Retinal Vein Occlusions,
Pseudo-exfoliation, Pigment Dispersion
Syndrome, etc.
|
 |
At what age does Glaucoma occur? |
| |
Mostly glaucoma
affect people in the fifth decade of their
life or later but it can occur at any age.
Glaucoma can occur even in young children
and infants (Developmental Glaucoma).
Occurring before the age of 3 years it is
called Congenital Glaucoma and between the
age of 3 and 30-35 years it is called Juvenile Glaucoma. Treatment of glaucoma is
more difficult in young patients and
operation is required more often. |
 |
What are the signs & symptoms? |
| |
Open angle type of
glaucoma usually does not give rise to any
symptoms in early stages. In late stages
patients may feel pain in eyes and
discomfort, and some individuals may notice
field defects (inability to see certain
areas of the field of vision). Usually this
type of glaucoma is diagnosed on examination
by a eye specialist either when he suspects
it because of some risk factors or during
the course during the course of a routine
examination.
Angle closure type of glaucoma can give rise
to pain in the eye and headache with
vomiting, seeing colored rings (haloes)
around lights and redness in the eyes
usually after coming out of a movie theatre.
This type of glaucoma may occur as sudden
attacks where there is severe pain in the
eye, redness, watering, vomiting and blurring of vision. |
 |
Can Glaucoma be treated? |
| |
Glaucoma can be
treated but the damage done by the disease
can not be reversed or undone. Further
damage to the eye by glaucoma can be
stopped. Therefore, it is of utmost
importance that the glaucoma be diagnosed
and treated early before significant damage
has been done. |
 |
How is Glaucoma and its
severity / damage diagnosed? |
| |
Following tests are
performed to diagnosed glaucoma, measure its
severity and the extent of damage:
- Intraocular
Pressure (Eye Pressure): Measured by an
instrument called Applanation Tonometer
(generally accepted as standard),
normally ranges between 11 and 21 mm Hg.
It may be modestly raised in open angle
glaucoma and markedly raised in angle
closure glaucoma. In between the attacks
of angle closure glaucoma it may be
normal. It may vary at different times
of the day and this variation can be
measured by noting pressures round the
clock at specified interval (Phasing /
Diurnal Variation). In low tension or
normal tension glaucoma the pressure may
never be higher than normal range.
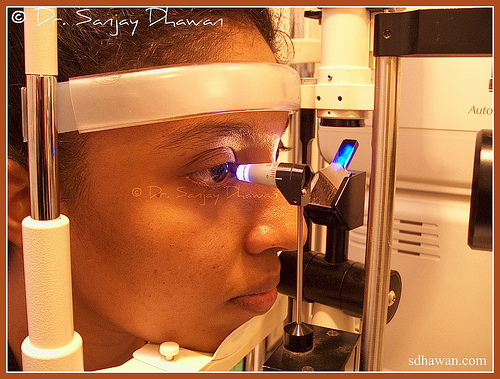
- Gonioscopy: A method to assess the angle of anterior
chamber of the eye. It helps in
diagnosing the type of glaucoma or even
the vulnerability of the person to have
attacks of angle closure glaucoma.
-
Fundus: The
retina and optic nerve of the eye can be
seen by an instrument called
ophthalmoscope. The optic disc undergoes characterstic changes in glaucoma which
are noted by measuring cup : disc ratio
or the C:D Ratio which is normally 0.3
to 0.4 and almost equal in both eyes. In
open angle glaucoma and later stages of
angle closure glaucoma it may be
increased. This increase is usually
proportionate to the extent of damage
done. However, in some normal
individuals also the C:D ratio may be
increased.
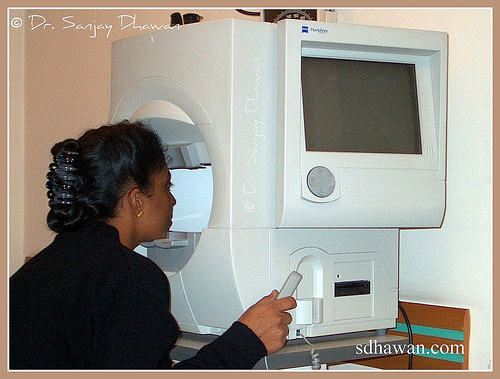
- Visual Fields: Simply stated it measures the "area of
vision" of a single eye, it also
measures the sensitivity of each point
in this area. Visual fields are now a
days charted by instrument called Computerized Automated Perimeter (Humphrey is generally accepted as
standard). In this test light patient is
shown light targets of various size and
brightness and note is made of the area
where the patient can see this. The data
thus collected is analysed and compared
with data of normal population. Glaucoma
gives rise to characteristic field
defects which progress in a peculiar
manner. This is the definitive test to
not only detect glaucoma but also assess
the severity and extent of damage. The
adequacy of the treatment is best judged
by visual field charting done at regular
intervals.
- OCT / HRT: Ocular Coherence Tomography (OCT) & Heidleberg Retinal Topography (HRT) are
sophisticated imaging techniques which
help in evaluation of optic nerve head &
retinal nerve fiber layer. They help in
objective quantification of the damage
caused to the nerve fibers.

|
 |
What is the treatment? |
| |
The treatment
options of glaucoma includes:
The treatment is
decided by many factors:
Decision
regarding what treatment and when to be
used should be left to the judgment of
consulting eye surgeon.
Detected early and
treated properly, glaucoma is perfectly
compatible with life long good vision. If
neglected it can end in blindness. |
 |
Discussion |
| |
What if a
person has both Cataract & Glaucoma?
Co-existence of glaucoma & cataract pose
difficulty in management of either. There is
always a dilemma whether to operate them
together or one at a time.
As a general principle, in cases of patient
with both Cataract & Glaucoma it is
desirable to control glaucoma first and then
proceed for cataract surgery. If the
pressure / glaucoma control is easily
achieved by 1-2 drugs then one can go for
cataract surgery without worrying about
glaucoma. In cases of advanced glaucoma or
when the pressure requires more than 2-3
drugs for control then one may have to
consider glaucoma surgery. Although it is
possible to do both glaucoma & cataract
surgery together at the same time, however,
the results may be slightly compromised. It
is ideal to do glaucoma surgery first and
cataract surgery later, if the clinical
condition of the eye & the patient permits.
Only in advanced glaucoma & advanced
cataract with impending complications, is it
justified to proceed with Combined Cataract
& Glaucoma Surgery also called Phaco-Trab or
Phacotrabeculectomy. |
